Published: 6 June 2013
Publications
NSAIDs and Acute Kidney Injury
Prescriber Update 34(2):14–15
June 2013
All non-steroidal anti-inflammatory drugs (NSAIDs) have been associated
with the development of acute kidney injury.
NSAIDs and Acute Kidney Injury
NSAIDs can cause two different forms of acute kidney injury1.
- Haemodynamically mediated (eg, pre-renal injury and/or acute tubular necrosis).
- Immune mediated (eg, acute interstitial nephritis).
Acute kidney injury represents a continuum of renal injury ranging from clinically asymptomatic changes in renal function to renal failure and death. Acute kidney injury is characterised by a rapid fall in glomerular filtration rate (GFR) over hours to days.
Presentation and Diagnosis
There are no specific signs or symptoms for NSAID induced acute kidney injury. Symptoms of acute kidney injury can be non-specific and may include shortness of breath, fatigue, confusion, nausea, decreased urine output and ankle/leg swelling2.
Patients with pre-renal injury may have signs of volume depletion (eg, tachycardia, absolute or postural hypotension, low jugular venous pressure, dry mucous membranes). Patients with interstitial nephritis may have features of a systemic hypersensitivity including fever, arthralgia and a pruritic erythematous rash. Eosinophilia may also be present.
Pathogenesis and Risk Factors
NSAIDs reversibly inhibit the production of renal prostaglandins via their inhibition of COX-1 and COX-2. Maximal inhibition occurs at steady state plasma concentrations (usually 3–7 days).
Renal prostaglandins cause dilatation of the renal afferent arteriole. This mechanism is important for maintaining GFR when renal blood flow is reduced (ie, not in young, healthy people)1. Therefore, NSAID use is likely to have a greater effect on renal function in patients with other risk factors (Table 1).
It is unclear how NSAIDs induce acute interstitial nephritis. However, it has been suggested that cyclooxygenase inhibition causes preferential conversion of arachidonic acid to leukotrienes, which may then activate helper T cells1.
Table 1: Risk factors for NSAID induced acute kidney injury1, 2
| Risk factor | Effect |
|---|---|
| Increasing age (particularly age >65), chronic hypertension and atherosclerosis | Narrowing of renal arterioles which may reduce their capacity for renal afferent dilatation |
| Pre-existing glomerular disease or renal insufficiency | Renal afferent dilatation is likely to be required to maintain GFR |
Volume depletion
|
Lowers afferent glomerular arteriolar pressure and stimulates secretion of angiotensin II |
| Use of ACE inhibitors or ARBs | ACE inhibitors and ARBs prevent efferent arteriole vasoconstriction which is also important in maintenance of GFR |
| Use of the 'triple whammy' (ACE inhibitor or ARB plus diuretic plus NSAID) | Diuretic may cause volume depletion. See above for ACE inhibitor/ARB effects. |
ACE=Angiotensin Converting Enzyme; ARB=Angiotensin II Receptor Blocker
Pre-existing chronic kidney disease and increasing age are the most common risk factors for developing acute kidney injury3.
The 'Triple Whammy'
A recent nested case-control study found that current use of triple therapy (ACE inhibitor/ ARB, diuretic and an NSAID) was associated with an increased rate of acute kidney injury (Rate Ratio 1.31, 95% CI 1.12–1.53) compared to double therapy (diuretic plus ACE inhibitor/ARB).
The greatest risk was observed in the first 30 days of use (Rate Ratio 1.82, 95% CI 1.35-2.46)4. This ‘triple whammy’ effect was first identified from case reports in early 2000 and was highlighted in Prescriber Update in 20025.
Treatment
Renal function will recover in most patients after withdrawal of NSAID therapy. Steroids may aid recovery in patients with interstitial nephritis who do not improve after stopping NSAID therapy. NSAID use should be avoided in the future in such patients1.
New Zealand Information
NSAIDs are indicated to relieve moderate pain and inflammation associated with conditions such as rheumatic disorders, surgery and/or dysmenorrhoea.
PHARMAC data indicates that ibuprofen is the most commonly prescribed NSAID in New Zealand. This is followed by diclofenac and naproxen.
The Centre for Adverse Reactions Monitoring (CARM) received 119 reports of renal adverse reactions associated with NSAID (including COX-2 inhibitor) use from 1 January 2000 (Figure 1).
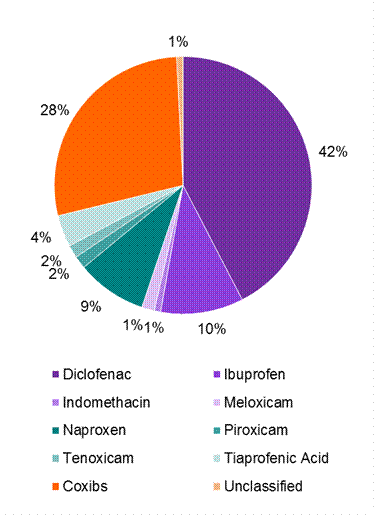
Figure 1: Renal adverse reaction reports from 1 January 2000 to 31 December 2012
Approximately 70% of reports were serious, including four deaths and 12 that were considered to be life-threatening. The majority of reports (74%) occurred in patients aged 50 years and over.
Diclofenac was the most commonly implicated NSAID (53 reports). In two thirds of the reports, other medicines were also considered suspect, including four reports that described the ‘triple whammy’. Reports included acute renal failure (33 reports), renal tubular necrosis (5) and interstitial nephritis (12).
Healthcare professionals are encourages to report suspected adverse reactions to NSAIDs to CARM.
References
- Rose BD, Post TW. 2013. NSAIDs: Acute kidney injury (acute renal failure) and nephrotic syndrome. In UpToDate, Basow, DS. (ed). Waltham: UpToDate. URL: www.uptodate.com (accessed 10 May 2013).
- Longo DL, Fauci AS, Kasper DL, et al. (eds). 2012. Harrison's Principles of Internal Medicine. New York: McGraw-Hill Education. URL: www.accessmedicine.com (accessed 10 May 2013).
- Best Practice Advocacy Centre. 2012. Acute-on-chronic kidney disease: prevention, diagnosis, management and referral in primary care. Best Practice Journal 46: 10–5. URL: www.bpac.org.nz/BPJ/BPJ.aspx (accessed 10 May 2013).
- Lapi F, Azoulay L, Yin H, et al. 2013. Concurrent use of diuretics, angiotensin converting enzyme inhibitors, and angiotensin receptor blockers with non-steroidal anti-inflammatory drugs and risk of acute kidney injury: nested case-control study. BMJ 346: e8525.
- Savage R. 2002. A Dangerous Trio. Prescriber Update 23(2): 20. URL: www.medsafe.govt.nz/profs/PUarticles/DangTrio.htm (accessed 23 May 2013).





